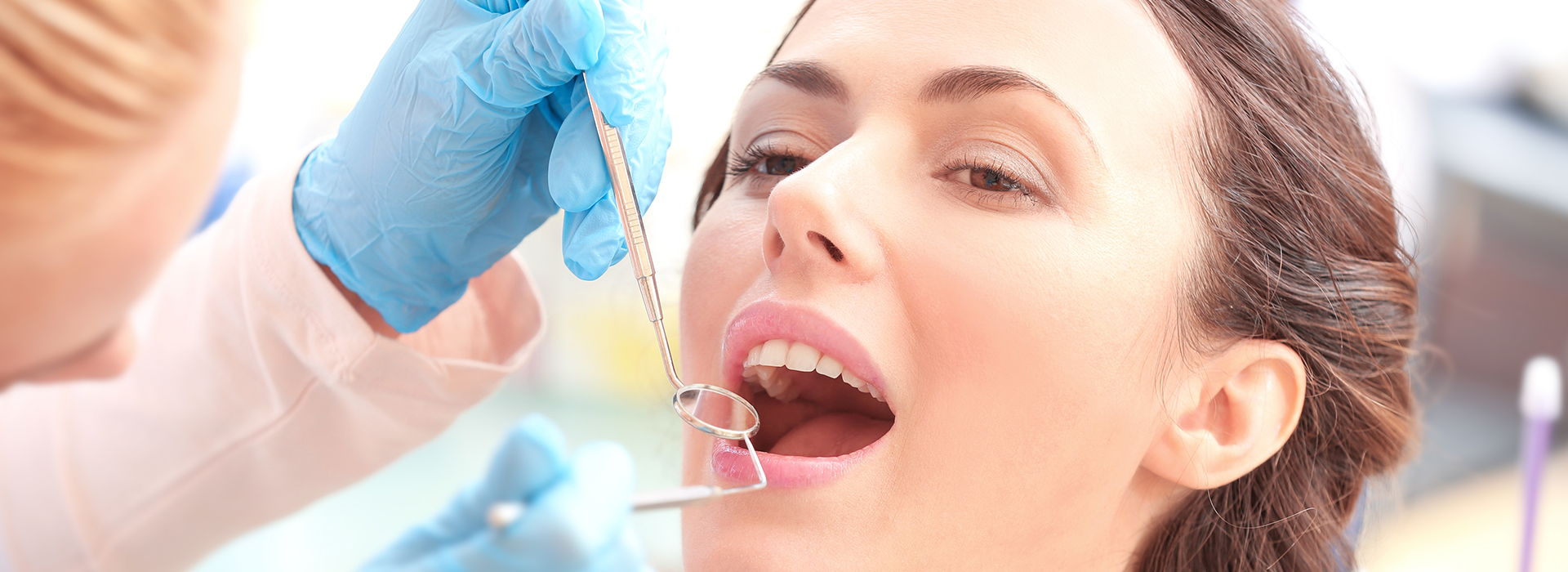
Gum disease is more common than many people realize. According to the Centers for Disease Control and Prevention, roughly half of adults over 30 in the United States show signs of periodontal disease. The condition ranges from mild, reversible inflammation to advanced tissue and bone loss that can threaten the long-term stability of the teeth. At the office of Park Dental Wellness, we focus on early detection, practical prevention, and evidence-based treatments that preserve oral health and function.
Periodontal disease begins when bacterial plaque builds up along the gumline and beneath the gums. The body’s immune response to that bacterial challenge causes inflammation in the soft tissues and, over time, can damage the connective tissues and bone that anchor teeth. Because the process often advances slowly and without obvious pain, regular dental exams are crucial to spot early warning signs.
Not all inflammation leads to irreversible damage. In its earliest phase, known as gingivitis, the problem is generally limited to the gum tissue and is fully recoverable with improved oral hygiene and professional care. When intervention is delayed, however, the disease can progress to periodontitis, at which point structural support for the teeth is at risk.
Understanding how the disease develops helps patients make smarter choices about daily care and professional treatment. Effective periodontal care targets the root causes—plaque, bacterial toxins, and pockets of infection—while supporting the body's efforts to heal and regenerate affected tissues.
Common signs that warrant a periodontal evaluation include:
Inflamed, swollen, or persistently red gums
Bleeding during brushing or flossing
Gum recession that exposes root surfaces
Increased tooth sensitivity to temperature or sweets
Chronic bad breath or a lingering unpleasant taste
Teeth that appear loose or a noticeable change in bite
New spaces developing between teeth or trouble with partial dentures fitting
Pus or other discharge around the gumline
Discomfort when chewing or biting that is not related to a cavity

Research increasingly shows that oral inflammation can influence overall health. Persistent periodontal infection is associated with higher inflammatory markers in the bloodstream and has been linked with conditions such as heart disease, diabetes, and certain respiratory illnesses. While the exact nature of these connections is complex, maintaining periodontal health is a sensible part of a broader strategy for general well-being.
Good gum care reduces bacterial load and inflammation locally, which in turn can lower the burden on the rest of the body. For people with chronic medical conditions—especially diabetes—controlling periodontal inflammation can make a meaningful difference in how well systemic conditions are managed.
Our clinical approach emphasizes prevention and coordination with patients’ broader healthcare needs. We aim to identify periodontal issues early and to recommend practical, sustainable treatments that support both oral and overall health.
Gingivitis is the name given to early-stage gum inflammation. It is typically limited to the soft tissue and does not involve irreversible bone loss. The signs are often subtle—slight bleeding with brushing, mild redness, or tender gums—but when caught early, gingivitis responds well to conservative measures.
A combination of improved home care—consistent brushing with a fluoride toothpaste, daily interdental cleaning, and antimicrobial rinsing when appropriate—along with professional cleanings can usually resolve gingivitis. Education and simple habit changes are powerful tools that prevent relapse and keep inflammation from advancing.
Regular follow-up and periodontal reevaluation are important after treatment. Even when symptoms improve, professional monitoring helps ensure pockets are shrinking and tissues are returning to a healthy state rather than masking a deeper problem.

If gingivitis is not adequately controlled, the disease can extend below the gumline and produce periodontitis. In this stage, bacteria and the inflammatory response begin to erode the connective tissues and the bone that hold teeth in place. Clinically, this is seen as deeper periodontal pockets, recession, and sometimes mobility of teeth.
The goals of care for periodontitis are to eliminate the pathogenic bacterial environment, reduce pocket depths to manageable levels, and preserve or rebuild the supporting structures whenever possible. Treatment is tailored to the severity and pattern of disease and often involves a staged plan of care that balances conservative measures with surgical or regenerative options when indicated.
Successful management combines meticulous mechanical cleaning, targeted antimicrobial strategies when needed, and an ongoing maintenance plan. Patients who understand their role in daily hygiene and follow clinical recommendations typically experience the best long-term outcomes.
Today’s periodontal care includes a spectrum of evidence-based options designed to stop disease and, where feasible, regenerate lost tissue. Non-surgical therapies, advanced antiseptic or localized antimicrobial techniques, laser-assisted treatments, and carefully planned surgical interventions are all part of modern practice.
Regenerative procedures—such as bone grafts, guided tissue regeneration, and biologic modifiers—can help rebuild supporting structures in areas where bone loss has occurred. These techniques are selected after a thorough assessment and are combined with strict plaque control and maintenance to protect the long-term results.
Our team uses proven technologies and clinical protocols to design individualized treatment plans. Whether the goal is to arrest disease progression, improve the appearance of the gumline, or create a stable foundation for restorative care, the emphasis is on predictable, conservative care whenever possible. At the office of Park Dental Wellness, we prioritize treatments that restore health and function with lasting results.
A periodontal treatment plan begins with a comprehensive exam that includes pocket depth measurements, assessment of bone levels when indicated, and a review of medical history and risk factors like smoking or diabetes. From there, clinicians describe the recommended sequence of care and what to expect at each step.
Non-surgical therapy typically serves as the first line of treatment. When pockets are shallow to moderate and tissues respond well, ongoing maintenance may be sufficient. If pockets remain deep or if there is significant structural loss, surgical interventions are considered to access infected areas, reduce pocket depths, and, when appropriate, restore lost tissue.
Throughout treatment and afterward, a customized maintenance schedule—often more frequent than standard recall visits—is essential to preserve gains and detect any early signs of recurrence. Patient engagement in daily hygiene and follow-up visits is the single most important factor in preventing disease progression.
When disease is detected early or when pockets are accessible with instruments, non-surgical treatment is the preferred starting point. Scaling and root planing remove plaque and hardened deposits below the gumline and smooth root surfaces so healing can occur. These procedures are often combined with improved home care instructions and selective use of local antiseptics or antibiotics.
The aim is to reduce inflammation, shrink periodontal pockets, and restore the gum tissue to a healthy attachment. For many patients, thorough non-surgical therapy followed by a disciplined maintenance program effectively controls the disease.
If non-surgical measures fail to produce adequate improvement, clinicians will consider additional interventions designed to reach areas that are not fully responsive to conservative care.
Surgery is recommended when pocket depths or the pattern of bone loss cannot be treated predictably with non-surgical approaches alone. Surgical techniques allow the clinician to thoroughly clean the roots and reshape the supporting bone. Flap procedures, for example, expose the root and bone so infected tissue can be removed and the area can be recontoured for better health and hygiene.
Where appropriate, regenerative therapies such as grafts or guided tissue regeneration can encourage the reformation of lost bone and connective tissue. Modern surgical care aims not only to arrest disease but also to restore a healthy architecture that is easier for patients to maintain.
Post-operative maintenance and careful hygiene are critical after any surgical or regenerative procedure to protect the healing tissues and support long-term success.
Periodontal health is a long-term commitment that blends professional care with daily habits. If you have noticed any of the signs described here or if you would like an assessment of your gum health, please contact us for more information about our approach and how we can help protect your smile.

Periodontal disease is an inflammatory condition that affects the gums and the bone that support the teeth. It ranges from reversible gingivitis to more advanced periodontitis that can undermine tooth stability. The process typically begins when bacterial plaque accumulates at the gumline and provokes a chronic immune response.
Left unchecked, inflammation can deepen into periodontal pockets and lead to connective tissue and bone loss, often progressing without obvious pain. Early detection through regular exams allows targeted care that can halt or slow tissue destruction. At Park Dental Wellness, our focus is on identifying problems early and matching treatment to the stage of disease.
Common early signs include gums that are red, swollen or that bleed when you brush or floss. You may also notice persistent bad breath, a metallic taste, or increased tooth sensitivity. These symptoms often precede more serious changes and should prompt a periodontal evaluation.
Recession of the gumline, new spaces between teeth, or a change in how teeth fit together are indications that the condition may be advancing. Pus, looseness, or discomfort when chewing are less common early but require immediate attention if present. Regular professional assessments help distinguish reversible inflammation from established disease.
Several factors increase the risk of developing periodontal disease, including tobacco use, poorly controlled diabetes, certain medications, and genetic susceptibility. Age and long-term plaque accumulation also contribute to higher prevalence among adults. Pregnancy and hormonal changes can temporarily increase gum inflammation.
A medical history that includes heart disease, autoimmune disorders, or conditions that suppress immunity can affect treatment planning and outcomes. Lifestyle factors such as stress, poor nutrition, and inadequate oral hygiene further raise risk. Discussing these elements with your dental team helps tailor a prevention and treatment strategy.
Diagnosis begins with a comprehensive clinical exam that measures pocket depths, checks for bleeding on probing, and assesses gum recession and tooth mobility. Radiographs are used when indicated to evaluate bone levels and detect areas of hidden bone loss. The clinician will also review your medical history and risk factors to form a complete picture.
Periodontal charting and photographic documentation help track changes over time and guide treatment decisions. In some cases saliva testing or bacterial sampling may be used to identify specific pathogens or monitor response to therapy. Together these diagnostic tools allow for a personalized treatment plan.
Non-surgical therapy is often the first line of care and includes professional scaling and root planing to remove plaque and calculus below the gumline. This mechanical cleaning smooths root surfaces so the gums can reattach and pockets can shrink. Clinicians may combine these procedures with targeted local antimicrobials when appropriate.
Adjunctive options such as antimicrobial rinses, locally delivered antibiotics, or laser-assisted decontamination can enhance bacterial control for selected cases. Success depends on thorough plaque control at home and close follow-up to assess healing. Most patients experience significant improvement with careful non-surgical management and ongoing maintenance.
Surgical or regenerative procedures are recommended when non-surgical approaches cannot adequately access deep pockets or correct advanced bone defects. Common surgical techniques include flap surgery to allow thorough root debridement and recontouring of bone for improved hygiene. Regenerative methods like bone grafts and guided tissue regeneration aim to restore lost supporting structures when feasible.
Surgical care is carefully planned to balance disease control with preservation of soft tissue and esthetics, and it often includes suturing and post-operative instructions to support healing. Biologic modifiers may be used in combination with grafting to encourage tissue regrowth in suitable cases. Close postoperative maintenance is essential to protect the results.
Periodontal inflammation has been linked with elevated systemic inflammatory markers and associations with conditions such as diabetes and cardiovascular disease. Controlling oral infection can reduce inflammation burden and may positively influence the management of some chronic medical conditions. While the exact nature of these relationships is still under study, improving gum health is an important component of overall wellness.
For patients with systemic conditions, coordination between dental and medical providers helps ensure safe, effective care and optimizes outcomes. Smoking cessation, glycemic control, and attention to nutrition are examples of measures that support both oral and general health. Your dental team can help you understand how periodontal care fits into your broader health plan.
After active therapy, effective maintenance includes a customized schedule of professional cleanings and periodontal reevaluations to monitor pocket depths, inflammation, and attachment levels. These visits are typically more frequent than routine dental checkups and focus on interrupting bacterial repopulation. Home care remains the foundation of long-term success and should be reinforced at maintenance appointments.
At Park Dental Wellness, we develop maintenance programs that reflect each patient's risk profile and response to treatment. Regular reinforcement of brushing technique, interdental cleaning, and lifestyle counseling such as smoking cessation helps protect the tissues and preserve treatment gains. Early detection of recurrence allows prompt retreatment and better prognosis.
Gingivitis is reversible with consistent, improved home care and professional cleanings when detected early. Brushing twice daily with a fluoride toothpaste, daily interdental cleaning, and appropriate antimicrobial rinses reduce plaque and inflammation. Patient education and behavior changes are powerful tools for preventing progression.
To prevent recurrence, maintain regular dental visits for monitoring and reinforce oral hygiene habits when needed. Addressing contributing factors such as tobacco use, uncontrolled diabetes, or medications that reduce saliva also reduces the likelihood of relapse. If inflammation returns despite good home care, seek a periodontal evaluation to reassess the treatment plan.
You should seek specialty periodontal care if you have progressive tooth mobility, persistent deep pockets despite non-surgical therapy, or complex bone defects that may benefit from regenerative procedures. A periodontist also manages patients preparing for dental implants or those with complicated medical histories affecting healing. Referral is appropriate whenever the level of disease requires advanced surgical or restorative coordination.
During a specialty consultation, the clinician will review prior therapy, perform a detailed assessment, and explain realistic goals and options for care. Treatment may be staged and coordinated with your general dentist to restore function and long-term stability. A collaborative approach ensures that periodontal needs are integrated with other dental and medical priorities.

At Park Dental Wellness, reaching us is simple. Whether you have questions about treatments or are ready to schedule your next visit, our friendly team is here to guide you every step of the way. Call, email, or use our convenient online form—we’ll make sure your experience is easy, comfortable, and tailored to your needs.
Start your journey to a healthier, more confident smile today!